The pattern of the iron study results is consistent with effects of chronic inflammation. Serum ferritin 195 microgram/L (N 40-260) Problems in interpretation of serum ferritin levels in relation to body iron storesĪ 23-year-old man with long-standing microcytic anaemia unresponsive to oral iron supplements: However, in patients with iron deficiency, some clinical states can distort the relationship by causing the level of ferritin in the serum to increase (Table 4), although it is very uncommon for it to exceed 100 microgram/L in patients with iron deficiency. A subnormal serum ferritin has a high degree of specificity for iron deficiency. Concentrations in postmenopausal females correspond to those in males of a similar age, and are lower in children. The normal range is 25-155 microgram/L in menstruating adult females, and 40-260 microgram/L in adult males. The normal range of ferritin in serum is dependent on several variables including methodology, age and sex. Ferritin thus represents the most sensitive index of early iron deficiency. Subnormal levels of ferritin can be detected when iron stores are exhausted, but before the serum iron level has become affected. Problems in interpretation of serum transferrin levels in relation to body iron stores – Concurrent acute or chronic inflammation – Recent iron medication, possibly unappreciated as a component in vitamins with mineral supplements Problems in interpretation of serum iron levels in relation to body iron stores Estimation of serum iron alone in the investigation of anaemia is consequently inadvisable. Unfortunately, a low serum iron level in this setting is frequently misinterpreted as evidence of iron deficiency, a major diagnostic error that can be avoided by simultaneous examination of the transferrin level, which in this context is subnormal or in the low normal range. The effect on iron and transferrin levels persists as long as the inflammatory process is sustained, and is classically associated with the development of anaemia of chronic disease. This response can produce a marked decrease within a day, especially in the serum iron level. The concentrations of iron and transferrin in the serum are significantly affected, and fall rapidly as part of the acute phase response after the onset of the inflammation irrespective of the status of the iron stores in the body. The diagnostic specificity of a low serum iron for iron deficiency is lost in the presence of inflammatory processes and certain other forms of chronic disease (Tables 2 and 3). A subnormal level of iron in association with a supranormal level of transferrin is very strong evidence of iron deficiency (Table 1). The concentration of transferrin rises under these circumstances towards, or above, the upper limit of the normal range. The serum (or plasma) iron concentration falls progressively below the normal range (14-32 micromol/L) when the amount of iron in the body decreases after the reserves of iron have become exhausted. Endoscopy is appropriate only if there is evidence of iron deficiency not explained by other causes, or highly suggestive clinical indications of gastrointestinal disease. However, currently available tests provide a reliable index of iron status sufficiently frequently that it is not appropriate to perform endoscopic examinations merely because a patient has anaemia, especially normocytic anaemia. This gives a more reliable overview of the situation than is provided by any individual test. The impact of these factors can be recognised by combining the results of currently available tests. This is important to recognise as such distorted results may give a misleading view of the patient's iron stores. The results of tests of iron status are relatively frequently distorted by other clinical factors. It can also occur in some patients with anaemia secondary to chronic infection, inflammation, or malignancy (anaemia of chronic disease), even though the majority of these patients have a normal mean corpuscular volume (MCV). 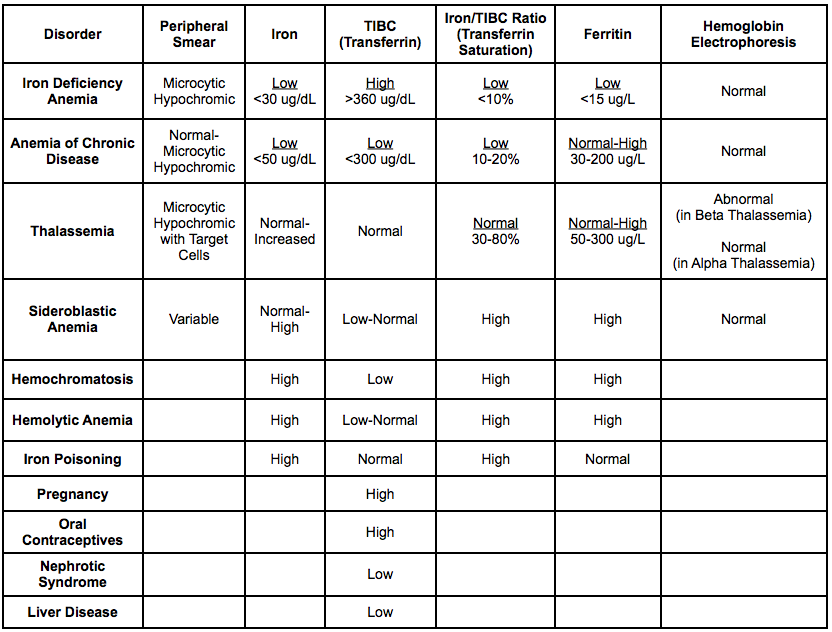
Microcytic anaemia is most commonly due to iron deficiency, but is also caused by thalassaemia. Biochemical tests for iron deficiency help to evaluate the cause of microcytic anaemia (a mean red cell corpuscular volume 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
